ORIGINAL RESEARCH
Predictors of Commercial Success in Blockchain Healthcare Insurance: A Mixed-Methods Analysis
Raaga Likhitha Musunuri, BDS, MS  ; Kimberly S. Brooks, MD, MS
; Kimberly S. Brooks, MD, MS  ; Swapna Ashish Patel, BPharm, MS
; Swapna Ashish Patel, BPharm, MS  ; Trupti Jayesh Majgunkar, MS
; Trupti Jayesh Majgunkar, MS  ; Krisha Patel, BS, MS
; Krisha Patel, BS, MS  ; and Erin O’Neill, MS
; and Erin O’Neill, MS 
Masters Students in Health Informatics, Bouvé College of Health Sciences and Khoury College of Computer Sciences, Northeastern University, Boston, Massachusetts, USA
Keywords: blockchain, commercial success, General Data Protection Regulation, healthcare insurance, Health Insurance Portability and Accountability Act of 1996, market capitalization, regulatory factors
Abstract
Background: Blockchain healthcare insurance offers substantial potential for improving data transparency, efficiency, and security. However, many blockchain healthcare projects struggle to scale up and achieve commercial success. Despite technical feasibility studies, limited research exists on the commercial success of these projects. This study explores the technical, regulatory, and strategic factors that contribute to market success in blockchain healthcare insurance initiatives.
Methods: Using exploratory mixed methods, we combined quantitative market data analysis from CoinGecko Application Programming Interface (API) with manual metadata curation from publicly available data. We conducted descriptive statistics, Pearson correlation, and multiple regression analysis to evaluate relationships between key variables and market success.
Results: The Health Insurance Portability and Accountability Act of 1996 (HIPAA) compliance emerged as a significant predictor of higher market cap (β = +12.6, p = 0.006), while insurance partnerships negatively impacted success due to early-stage complexity (β = –15.3, p = 0.009). The model explains 95.7% of market cap variance (adjusted R² = 0.957).
Findings: These findings demonstrate how crucial technical preparedness and regulatory alignment are to the successful commercialization of blockchain-based health insurance. The importance of organizational scale is highlighted by a moderate association (r = 0.83) between team size and market success. The importance of strategic alliances and regulatory compliance is further shown by the theme analysis of white papers. Investors should concentrate on projects with well-defined regulatory policies, while entrepreneurs should give HIPAA compliance top priority early on. It is recommended that policymakers create more precise regulatory frameworks for blockchain in the medical field. For more thorough insights, future studies should increase the sample size.
Plain Language Summary
Blockchain technologies have the potential to transform healthcare insurance by improving data security, transparency, and efficiency. However, many blockchain healthcare projects struggle to progress beyond the pilot stage. Our study explored factors influencing the market success of blockchain healthcare insurance projects, revealing that compliance with the Health Insurance Portability and Accountability Act of 1996 (HIPAA) and regulatory standards are key predictors of success. Additionally, having too many early-stage partnerships can hinder progress, while strategic partnerships are more beneficial. Larger project teams lead to better market performance. Entrepreneurs should prioritize regulatory compliance, and policymakers should establish clearer blockchain frameworks. These factors are crucial for both technical functionality and commercial viability.
Citation: Blockchain in Healthcare Today 2025, 8: 401.
DOI: https://doi.org/10.30953/bhty.v8.401
Copyright: © 2025 This is an open access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.
The authors of this article own the copyright.
Submitted: April 28, 2025; Accepted: July 8, 2025; Published: August 1, 2025
Corresponding Author: Raaga Likhitha Musunuri, Email: dr.raagalikhitha@gmail.com
Competing interests and funding: This editorial received no external funding.
As the 21st century began, the healthcare sector faced enormous pressure to offer high-quality services while keeping costs in check. Blockchain has evolved into a promising approach for implementing a distributed and secure healthcare data management and sharing service. From a conceptual standpoint, blockchain can be viewed as a distributed collaborative system upheld by various entities in an environment where trust cannot be assumed.
Blockchain enables secure data processing among multiple parties without the need for trusted third parties. Secure data processing among multiple parties can occur, and since the launch of Bitcoin in 2008, blockchain has garnered intense focus from academia and industry. Financial projections based on research and from markets indicate substantial growth in this sector, with the global blockchain market expected to expand from approximately $17.21 billion (€15.45 billion) in 2023 to $29.35 billion (€26.35 billion) in 2024, reflecting a compound annual growth rate of 70.6%.
This revolutionary approach to data security and verification is transforming sectors where privacy and integrity are paramount. Due to its outstanding characteristics, such as data traceability, tamper-proof data storage, and service availability, blockchain-based healthcare data management has been the subject of extensive research. With the addition of access control mechanisms, blockchain-based solutions enable flexible data sharing, promote accountability, and guarantee data authentication. As an example, Patientory (PTOY) leverages blockchain technology for storage and transfer of healthcare data, which guarantees secure and efficient data exchange.1
Health insurance represents a critical domain where blockchain’s transformative potential is particularly significant. The current healthcare insurance framework faces substantial challenges such as claim fraud, data security, interoperability, and trust challenges. The financial impact of these fraudulent activities is staggering, with estimates suggesting that healthcare fraud diverts approximately 10% of global healthcare spending, threatening economic stability worldwide.
Despite extensive research, the healthcare insurance industry still lacks real-time, comprehensive solutions for analyzing complex data from diverse sources. Blockchain technology combined with ensemble learning offers a promising solution through its decentralized, tamper-resistant ledger, enhanced security, and smart contract capabilities. By distributing patient data across networks, blockchain reduces centralized system risks while ensuring data immutability creates verifiable, unalterable medical records.2
However, there is a critical research gap between technical feasibility and commercial success in real-world implementations. Studies reveal that commercially successful blockchain healthcare projects represent merely 0.24% of tracked blockchain initiatives, as highlighted by Fang3 with most enterprise efforts remaining confined to exploratory groups and not progressing beyond pilots or limited trials into mainstream adoption, as emphasized by Krishnasamy and Gopalakrishnan.4 This research addresses the critical commercialization gap in blockchain healthcare insurance by investigating which factors meaningfully differentiate market-successful implementations from failed initiatives. Our research moves beyond theoretical feasibility to examine concrete determinants of commercial viability.
To fill the research gap in understanding what makes blockchain healthcare insurance projects successful, the important factors were grouped into three main categories: technical, regulatory, and strategic. We developed a conceptual framework (Figure 1) to address this identified research gap in commercialization success factors for blockchain healthcare insurance projects, emphasizing real-world implementations rather than merely theoretical possibilities. Our framework synthesizes insights from previous blockchain healthcare adoption studies3,4 while explicitly focusing on market success rather than implementation feasibility.
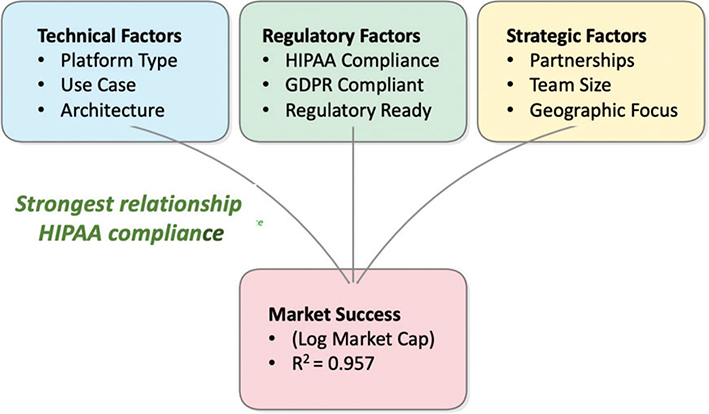
Fig. 1. Conceptual framework of determinants of success in blockchain health insurance. HIPAA: Health Insurance Portability and Accountability Act of 1996; EDPR: ElcomSoft Distributed Password Recovery (software).
Technical factors include the underlying blockchain platform (e.g., Ethereum vs. custom solutions), specific use case orientation (e.g., insurance claims processing vs. patient record management), and system architecture design. Regulatory factors center on compliance readiness, particularly adherence to the General Data Protection Regulation (GDPR) and the HIPAA, which may serve as critical signals of institutional trustworthiness and market credibility. Strategic factors encompass organizational characteristics such as the number and quality of partnerships, team size, and geographic focus.
These connected factors together affect how the market views a project, how ready institutions are to adopt it, and how it stands against competitors, which ultimately impacts the project’s success in the market, measured here as log-transformed market capitalization. Based on earlier research that highlights the importance of trust in regulations for adopting blockchain, we suggest that regulatory factors, especially HIPAA compliance, might have the biggest impact on a project’s success in the market, possibly accounting for major differences in how well it commercializes.
Literature Review
Contemporary healthcare insurance systems face mounting challenges from fragmented data architectures that impede effective information exchange and create vulnerabilities to widespread fraud. This fragmentation manifests as siloed patient information across providers and insurers, generating significant interoperability issues as disparate systems employ incompatible data formats and standards.
The financial impact of these systematic weaknesses is staggering. Medical identity theft alone costs the healthcare industry over $30 billion (€27 billion) annually, while healthcare fraud schemes worldwide result in approximate losses of $260 billion (€233 billion) to medical insurance funds. These figures highlight the urgent need for innovative approaches to manage healthcare insurance data that address interoperability and security concerns. The scope and variety of healthcare insurance fraud further highlight this pressing challenge. In 2016, a significant federal investigation resulted in charges against more than 300 healthcare professionals involved in fraudulent billing schemes totaling approximately $900 million (€807 billion).5
Beyond financial fraud, practices such as inappropriate opioid prescribing, often incentivized by deceptive pharmaceutical marketing campaigns that minimize addiction risks, compromise patient safety. These fraudulent activities collectively threaten the financial sustainability of healthcare insurance systems and patient well-being, creating momentum for technological solutions that can enhance transparency, security, and trust across the healthcare insurance ecosystem while preserving appropriate privacy protections.
The evolution of healthcare reimbursement models introduced new complexities in fraud detection. Traditional item-based payment systems have gradually shifted toward diagnosis-based models such as Diagnosis-Related Groups (DRGs), where insurers pay fixed amounts based on diagnostic categories rather than individual services rendered. While this approach helps control excessive medical treatment and rising costs by standardizing payments, it also creates new avenues for fraud through diagnostic code manipulation. Healthcare providers may intentionally upgrade low-cost disease codes to higher-paying alternatives to maximize reimbursement. The sheer volume of patient cases, with some Chinese provinces processing 15 million inpatients annually, makes manual auditing impractical, necessitating advanced technological solutions that can efficiently identify suspicious patterns while maintaining data integrity across the healthcare insurance ecosystem.6
Blockchain serves as a distributed solution to the growing complexity of healthcare data, offering real-time analysis, traceability, and counterfeit resistance.20 The immutable ledger and cryptographic protections of this system are ideal for the insurance sector, where data integrity and audibility are essential.1 By identifying unusual claim trends automatically, blockchain-enabled fraud detection systems enable proactive interventions, thereby preserving data privacy. Nevertheless, the adoption of blockchain in health insurance is inconsistent due to regulatory misalignment and technological innovation.2 Only 0.24% of blockchain ventures in the healthcare sector achieved commercial viability, primarily due to regulatory uncertainties and limited ecosystem integration.3
Healthcare data are subject to privacy regulations like HIPAA, and projects that prioritize regulatory alignment and confidentiality are more likely to gain institutional trust and be successful.7 Integrating decentralized identification systems with compliant blockchain frameworks elevates patient autonomy, privacy, and trustworthiness, which are key factors concerning the uptake of healthcare. However, the fragmented regulatory environment and absence of interoperability standards pose significant challenges to institutional adoption and scalability in healthcare blockchain endeavors.8
According to studies on blockchain healthcare insurance initiatives, team size and strategy alignment are critical factors. The lack of resources or an extremely limited focus tends to make teams unable to secure and sustain ongoing development and scaling.8 Conversely, larger, multidisciplinary teams are generally better attuned to address technical, legal, and regulatory issues associated with products.2 Collaborations among providers, regulators, insurers, and other stakeholders are essential for the success of programs. Excessive early-stage insurance partnerships can complicate operations and postpone financial returns.9 The results of literature studies indicate that strategic quality is more significant than quantity in these programs. Blockchain offers a workable answer to the problems that healthcare insurance systems face, including fraud, data fragmentation, and compliance, but only if technical implementation, regulatory alignment, and organizational maturity all line up.
Methods and Findings
Study Design and Rationale
This study uses a combination of methods (e.g., looking at numbers from the market and gathering information by hand) to understand what makes blockchain healthcare insurance projects successful (Figure 2). The market data help us see how successful the market is (e.g., market cap), while manually pulling information from white papers adds important details about things like rules and partnerships, which are key to understanding how blockchain healthcare insurance projects work. Prior research focused on the technical feasibility of the blockchain in healthcare, while the market success factors remain understudied and unclear.
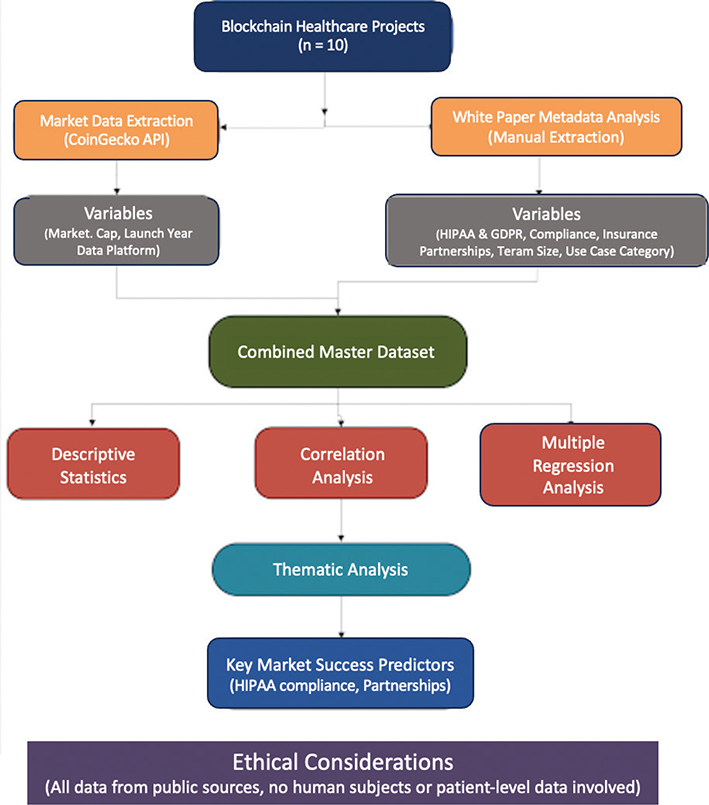
Fig. 2. Mixed methods methodology. HIPAA: Health Insurance Portability and Accountability Act of 1996.
Our study aims to do an exploratory analysis of the regulatory, technical, and strategic implications that enable market success and adaptability, such as the role of HIPAA compliance and partnerships with insurance companies.
Data Sources and Collection
The primary data sources include market data from the CoinGecko API (https://www.coingecko.com/en/ap) and publicly available white papers and project documentation (snapshot collected on April 20, 2025). The data retrieval used the standardized /coins/markets and /coins/id endpoints, extracting project-level information including market capitalization (US dollars), current trading volume, circulating supply, launch year (genesis date), and platform type. Retrieved data were saved in Comma-Separated Values (CSV) format and processed in Python (pandas v2.2.1). In addition to market data, metadata was manually extracted from the white papers and public documentation of the selected blockchain healthcare insurance projects. These documents provided valuable insights into various factors influencing the market success of these projects, including technical architecture, regulatory compliance, and strategic focus. The metadata collected focused on several key variables: HIPAA compliance, GDPR compliance, partnerships, platform type, use case, and team size.
Sampling Strategy
A purposive sampling method was used to select 10 blockchain healthcare insurance projects. The selection was based on the availability of white papers, market presence, and relevance to the healthcare insurance sector. Projects were included if they had publicly available white papers and market data, such as market cap and trading volume. Additionally, the projects selected were operational or had a visible market presence, indicating they were beyond the proof-of-concept phase.
Defining a Successful Project
The sample captured a cross-section of geographically diverse, thematically varied, and technically distinct projects in the blockchain healthcare ecosystem, despite its small size, which limits generalizability. But it was appropriate for an exploratory analysis in a niche and evolving sector. The HIPAA compliance was assessed as a critical factor in determining whether the project adheres to United States health information privacy standards.10 Compliance with GDPR was considered for projects operating in European markets, ensuring they meet the data protection and privacy regulations.11 The nature of partnerships with insurance companies, healthcare providers, and other relevant organizations was examined, as these partnerships can enhance the project’s credibility and integration into the healthcare system.
While HIPAA compliance was evaluated for projects targeting the US market and GDPR for those operating in Europe, other relevant data protection laws such as the California Consumer Privacy Act (CPRA) were not systematically included in this analysis; future research should expand the regulatory scope to capture additional regional frameworks.
The type of blockchain platform used by the projects was also documented, as it influences scalability, security, and interoperability. The use case of each project was also recorded to determine whether it focuses on insurance claims processing, medical record management, or another aspect of healthcare insurance. Finally, team size was noted as it could correlate with the project’s ability to scale and deliver successful outcomes.
Data Processing and Statistical Analysis
Key variables were “cleansed” (identify and resolve potential data inconsistencies or errors) and standardized. The dependent variable, market capitalization, was log-transformed (log1p) to normalize skewness, as raw market caps varied widely across projects. The study used several statistical methods for data analysis and was conducted using Python (pandas, statsmodels, and seaborn libraries). Descriptive statistics were calculated to summarize the key characteristics of the selected projects, including market cap, team size, and compliance rates. Pearson correlation coefficients were computed to explore the relationships between different variables, such as team size and market cap or HIPAA compliance and market success. Multiple regression analysis was also conducted using log-transformed market cap as the dependent variable. This method allowed for the evaluation of how different independent variables contributed to market cap while controlling for the influence of other variables. The log transformation of market cap was necessary to normalize the data, as market caps can vary significantly across projects.
Analyses were performed using Python libraries: statsmodels (v0.14.0) for regression modeling and SciPy (v1.14.1) for correlation analysis. Visualization of key findings was performed using matplotlib (v3.10.0) and Seaborn (v0.13.2). The use of mixed methods in this study is crucial to understanding the factors influencing market success. Quantitative data, such as market caps, alone would miss the critical business, technical, and regulatory context that is essential for understanding why certain projects succeed or fail. Manual metadata extraction from white papers and documentation provided important contextual information regarding the organizational, strategic, and regulatory dimensions of the projects, which could not be captured by market data alone. Market data collected from CoinGecko was validated against secondary sources (e.g., CoinMarketCap) to ensure accuracy within a 5% threshold.
Thematic Analysis Methodology
This study also used a thematic analysis to qualitatively assess the white papers and public documents of selected (n = 10) blockchain healthcare insurance projects, which helped us understand the organizational, strategic, and regulatory factors that may not be captured through quantitative market data alone. To achieve this, we collected the data from the white papers and public project documentation, which primarily had insights about various factors such as technical architecture, partnerships, regulatory compliance, and strategic focus that added insights on market success.
After this, we systematically coded these white papers using a deductive approach, which was derived from our research questions and literature review. This included categories such as regulatory compliance (e.g., HIPAA, GDPR), partnerships (with healthcare providers, insurers, etc.), platform type (Ethereum, custom, etc.), tokenomics (utility, rewards systems), and data privacy and artificial intelligence (AI) focus. This also involved identifying references to these themes within the white papers and assigning corresponding codes. For example, a reference to HIPAA compliance in a white paper was coded under the regulatory compliance theme, and other such things.
Two independent researchers conducted the coding process, ensuring the reliability and consistency of the results. Any discrepancies were discussed and resolved through consensus. This process aimed to minimize coding bias and improve the accuracy of the analysis. After the initial coding, themes were further refined and categorized into broader patterns of strategic focus. For example, partnerships were further divided into strategic partnerships with healthcare providers, insurance partnerships, and other partnerships (e.g., technology partners and investors). Two independent researchers reviewed manual metadata coding to ensure consistency. Discrepancies were resolved through consensus discussion. Reliability metrics (e.g., inter-rater agreement) are reported in Appendix A. This process minimized errors and ensured the data’s accuracy. However, future research should apply structured coding frameworks to standardize the extraction and analysis of metadata, which would further improve the reproducibility of the study and reduce potential biases introduced by manual data collection. The themes were analyzed to identify the most influential factors impacting market success. These insights were then triangulated with quantitative data (e.g., regression results, correlations) to provide a more comprehensive understanding of the factors contributing to market success.
Methodological Challenges
The primary methodological challenges that arose were handling multicollinearity and bias minimization. Moderate multicollinearity was detected (e.g., HIPAA compliance variance inflation factors [VIF] ≈ 9) which was addressed through careful interpretation of coefficients and acknowledging limitations in extrapolation beyond exploratory findings. Manual metadata extraction was standardized through predefined coding categories. Sampling bias was minimized by adhering to explicit project selection criteria. In addition, keeping the market data volatility in mind, all the CoinGecko data was collected within the same 1-week window (April 2025) to control cryptocurrency market fluctuations.
Ethical Considerations
All data utilized were publicly available through open-access sources. No human subjects or patient-level data were involved. Institutional Review Board (IRB) approval was not required.
Results
Descriptive Statistics and Project Characteristics
Table 1 presents the descriptive statistics for the 10 blockchain healthcare insurance projects included in this study. The table includes various factors such as market cap, team size, HIPAA compliance, GDPR compliance, and insurance partnerships, which helped in understanding the interdependencies that affect the performance of these projects in the market. The projects exhibit considerable variation in market capitalization, with a mean of $3.76 million (standard deviation [SD] = 3.04) and a range from $0.3 to $8.2 million. Team sizes averaged 43.5 members (SD = 24.27), ranging from small teams of 10 to larger organizations with 80 members. Half of the analyzed projects demonstrated HIPAA compliance, while a larger proportion (80%) were GDPR-compliant. The projects maintained an average of 1.5 insurance partnerships (SD = 1.08), ranging from 0 to 3 partnerships.
Market Capitalization Distribution
As seen in Figure 3, the market capitalization distribution is heavily skewed, with MediBloc (MED), a blockchain healthcare platform for secure medical data management, dominating the chart. This supports the finding of regulatory compliance being a significant success factor, as MED was one of the projects with the highest compliance and market cap, with close to $74.5 million (€66.73 million), substantially outperforming other projects in the sample. Interestingly, as we can see from Figure 3, there is no active market value, despite technical prowess and promise in projects like Humanscape (HUM), a patient-centered blockchain healthcare ecosystem, Doc.com (MTC), a blockchain-based telemedicine platform, Lympo (LYM), a blockchain-based health and wellness platform with incentivized fitness activities, AI Doctor (AIDOC), a blockchain-based healthcare platform using AI for medical diagnostics, and Remote Patient Monitoring (RPM) applications. This points to the significant challenges faced by many blockchain healthcare initiatives in achieving substantial market traction. This skewed distribution emphasizes the finding that successful projects possess distinctive characteristics that separate them from less successful counterparts in this emerging sector.
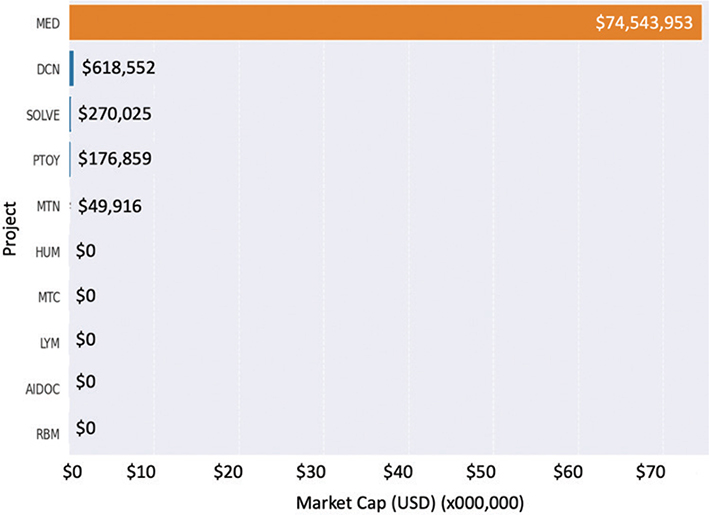
Fig. 3. Market capitalization. AIDOC: AI Doctor; LYM: Lympo; MED: MediBloc; MTC: Doc.com; MTN: Medicalchain; HUM: Humanscape; PTOY: Patientory; RBM: Robomed Network; SOLVE: Solve.Care; USD: US dollars.
The correlation matrix visually represented in Figure 4 reveals important relationships between key variables in our study. As observed in the figure, there is a strong positive correlation between HIPAA compliance and market capitalization (r = 0.81), which indicates that regulatory compliance is one of the primary factors that drive a blockchain health insurance project’s success. Team size also showed a remarkable correlation with market capitalization (r = 0.83), suggesting that organizational scale contributes to project success, as they might provide a better competitive edge. Insurance partnerships displayed a moderately strong correlation with market capitalization (r = 0.71), highlighting the importance of strategic alliances in achieving market success.
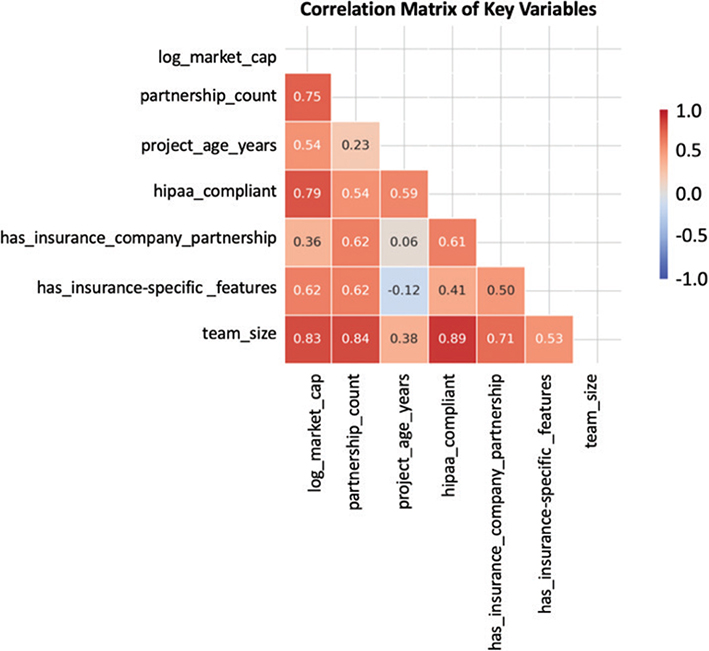
Fig. 4. Correlation heatmap. HIPAA: Health Insurance Portability and Accountability Act of 1996.
Interestingly, GDPR compliance showed a weak correlation with market capitalization (r = 0.05), suggesting that while European data protection regulations may be important for global operations, they appear to have less direct impact on market success compared to US healthcare regulations in this sample. However, GDPR compliance showed moderate correlations with team size (r = 0.51) and insurance partnerships (r = 0.49), which may indicate indirect effects on market performance through organizational maturity and partnership development.
HIPAA Compliance and Market Success
As observed in Figure 5, HIPAA compliance played a major influence on market success with these projects. HIPAA-compliant projects showed a higher market capitalization compared to non-compliant counterparts. This also strongly supports our regression findings, which identified HIPAA compliance as a significant positive predictor of market success (β = 12.6, p = 0.006). The distinct statistical significance that this relation has shown is that regulatory compliance is critical for blockchain healthcare projects. The compliant projects had nearly 12.6 times higher market capitalization than those that do not. This reiterates that regulatory trust and institutionality are important in the healthcare blockchain sector.
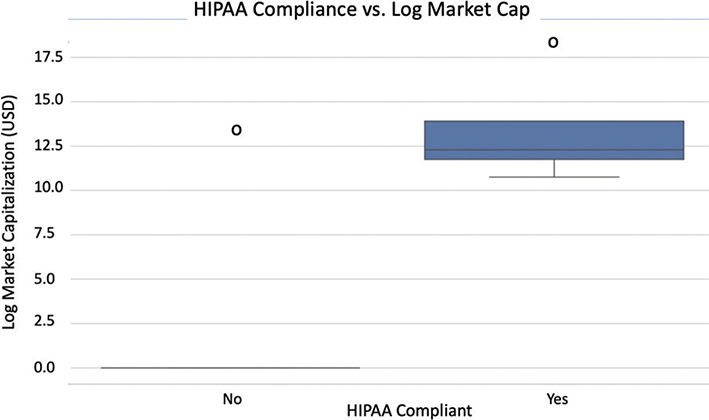
Fig. 5. HIPAA Compliance versus Log Market Cap Boxplot. HIPAA: Health Insurance Portability and Accountability Act of 1996; USD: US dollars.
Insurance Partnerships and Market Performance
In addition, when we look at insurance partnerships and market capitalization, there are further interesting relationships that emerge (Figure 6). The scatterplot shows an overall moderate positive correlation with r = 0.61; it also shows reduced returns, which resulted out of operational complexity from too many partnerships, and there are few other projects with higher returns despite lower partnership numbers. This could mean that while partnerships enhance and improve a project’s market outcomes, strategic alignment and quality are more important than numbers. This is also substantiated by our findings from regression analysis which showed a negative correlation between insurance partnerships and market success, when we controlled for other variables (β = –15.3, p = 0.009). In addition to this, it could be plausible that projects that had numerous early-stage partnerships might have faced operational complexity without immediate financial returns, which often ends up delaying the project’s ability to scale and further impact its market growth.
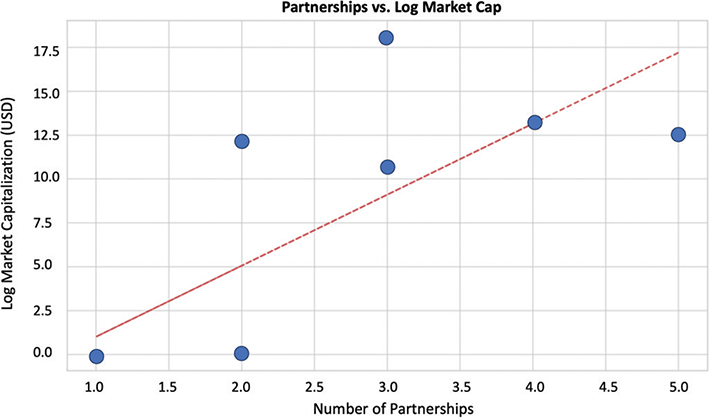
Fig. 6. Partnerships versus market cap scatter plot. USD: US dollars.
Confluence of Compliance and Partnerships
Figure 7 shows the combined effect of HIPAA compliance and strategic partnerships that affect market success. As observed in projects such as MED and Medicalchain (MTN), a blockchain platform for secure electronic health record management, which are HIPAA-compliant with multiple partnerships at the top-right quadrant, they show a simple, straightforward correlation of market success. On the other hand, other projects, such as Robomed Network (RBM), a blockchain platform connecting healthcare providers and patients using smart contracts, AIDOC, and Doc.com (MTC), either lack compliance or rely solely on partnerships or are located in the lower quadrants with weaker market caps. The positioning of projects like MED and Solve.Care (SOLVE), a blockchain platform for healthcare administration and payments, in the right quadrant confirms their superior market performance backed by both regulatory compliance and strategic partnership development. This reiterates the idea that market success is not just determined by the number of partnerships but by a combination of regulatory readiness and strategic alliances. Projects that focus on both compliance and meaningful partnerships appear to be more successful in capturing market value.
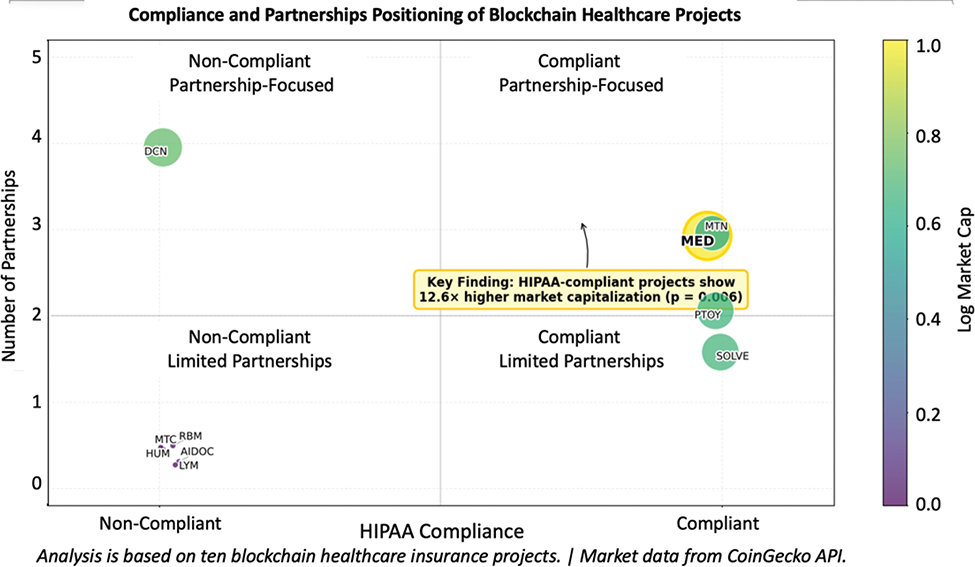
Fig. 7. Compliance and partnerships quadrant bubble chart. AIDOC: AI Doctor; DCN: Dentacoin (blockchain platform focused on dental healthcare); HIPAA: Health Insurance Portability and Accountability Act of 1996; HUM: Humanscape; LYM: Lympo; MED: MediBloc; MTC: Doc.com; MTN: Medicalchain; PTOY: Patientory; RBM: Robomed Network; SOLVE: Solve.Care.
Temporal Analysis of Project Launch Year and Market Success
The next part of our analysis relates to the project launch year and market success relations, where we identified that the earlier launched projects (2015–2016) achieved a higher market capitalization than later entrants (2017 and beyond). The early market entry provided a first-mover advantage to these projects. In the project PTOY, a blockchain healthcare platform for patient-controlled health data management, which was launched in 2017, strategic execution and regulatory compliance were likely more significant factors in its market performance than simply being an early entrant, which implies that this is not a deterministic relationship. The trend line in Figure 8, with a correlation of r = 0.24, suggests a mild relationship between earlier launch years and market success. However, it highlights that the quality of execution remains crucial for long-term success. This finding indicates that while being an early mover provides certain advantages in the blockchain healthcare space, project longevity alone does not guarantee commercial success without proper regulatory alignment and strategic execution.
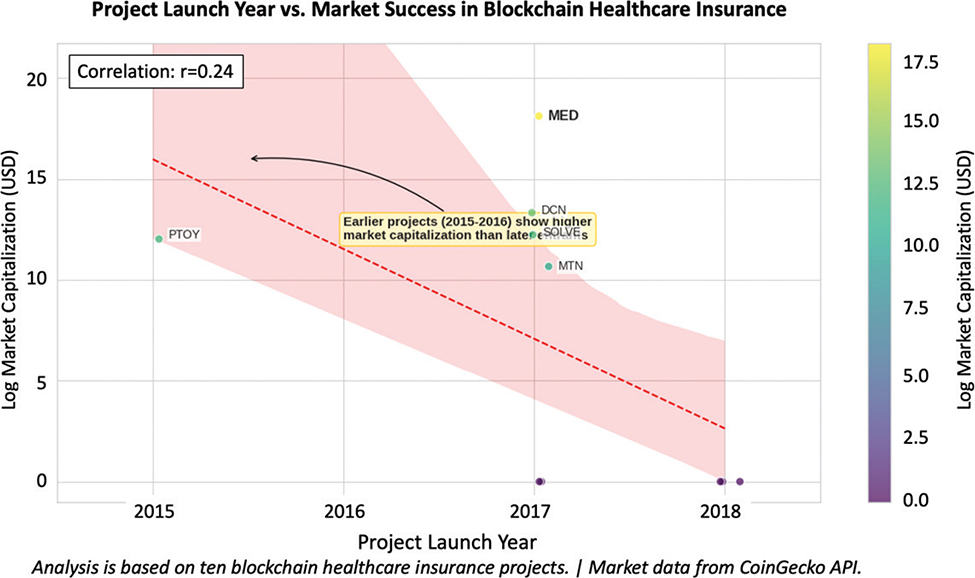
Fig. 8. Project timeline: launch year vs. current market status. MED: MediBloc; DCN: Dentacoin; MTN: Medicalchain; PTOY: Patientory; SOLVE: Solve.Care.
Thematic Analysis of White Papers
Our thematic analysis of blockchain healthcare insurance project white papers revealed several key themes that influence market success. Table 2 summarizes these themes and the supporting evidence from our data analysis.
The quantitative findings were reiterated by the thematic analysis we conducted, during which we identified more nuanced insights about regulatory compliance, partnership strategy, platform choice, use case, tokenomics, and AI/data privacy. During the analysis, we found that HIPAA compliance is a defining theme among leading projects. HIPAA-compliant projects are strongly associated with higher market capitalization, as shown by both correlation (r = 0.79) and regression analysis (β = 12.63, p = 0.006). This suggests that regulatory alignment is not only a technical or legal checkbox but a key market signal for trust and adoption in blockchain healthcare. A couple of projects, such as Solve Care and MED, highlighted HIPAA compliance as a key driver of their success, ensuring that their platforms gained trust and institutional adoption.
The number of partnerships is positively correlated with market capitalization (r = 0.75), highlighting that ecosystem integration and external collaborations are central to project visibility and value. Projects with more partnerships tend to have greater resources, reach, and legitimacy, which translates into higher market cap. MED, for example, formed a key partnership with South Korean healthcare providers, boosting its market credibility. However, partnerships specifically with insurance companies showed a negative association with market cap in regression (β = –15.11, p = 0.009). This unexpected finding may reflect the challenges and slow pace of insurance sector adoption or that insurance-focused partnerships alone do not guarantee broader market traction. Team size is another strong theme that we identified, which was reinforced from quantitative insights, where we saw larger teams are associated with higher market capitalization (correlation r = 0.83). This suggests that organizational capacity – reflected in human resources – enables better execution, product development, and market engagement.
Our thematic analysis also revealed that most of the projects use Ethereum or custom blockchain platforms, which employ dual or multichain architectures, but this was not a significant predictor in our regression analysis, which implies that for this sample, technical stack alone is not a differentiator for market success. Another significant finding from this analysis is that projects like MED migrated from Qtum/Ethereum to their custom “Panacea” blockchain to improve scalability and interoperability. This revealed that the interoperability with existing healthcare systems, such as electronic health records (EHR) integration, was a stronger predictor of success than just the choice of platform.
Another key factor identified was data privacy and AI diagnostics, as in the case of PTOY and tokenomics in the case of Dentacoin. This had less impact on market success, which implies that data ownership and privacy in the healthcare space are more valued than rewards. Finally, from our thematic analysis, we identified that projects spanned across different use cases (insurance, personal health records, dental, wellness, diagnostics, claims) and geographic focuses (Global, US, Asia, Europe). Dummy variable analysis and regression suggest that global focus may have a borderline positive effect (β = 8.84, p = 0.057), but use case category and platform are not statistically significant predictors. The correlation heatmap reveals that HIPAA compliance, team size, and partnerships are themselves interrelated, reflecting that successful projects tend to align across multiple strategic and organizational dimensions.
Regression Analysis and Multicollinearity
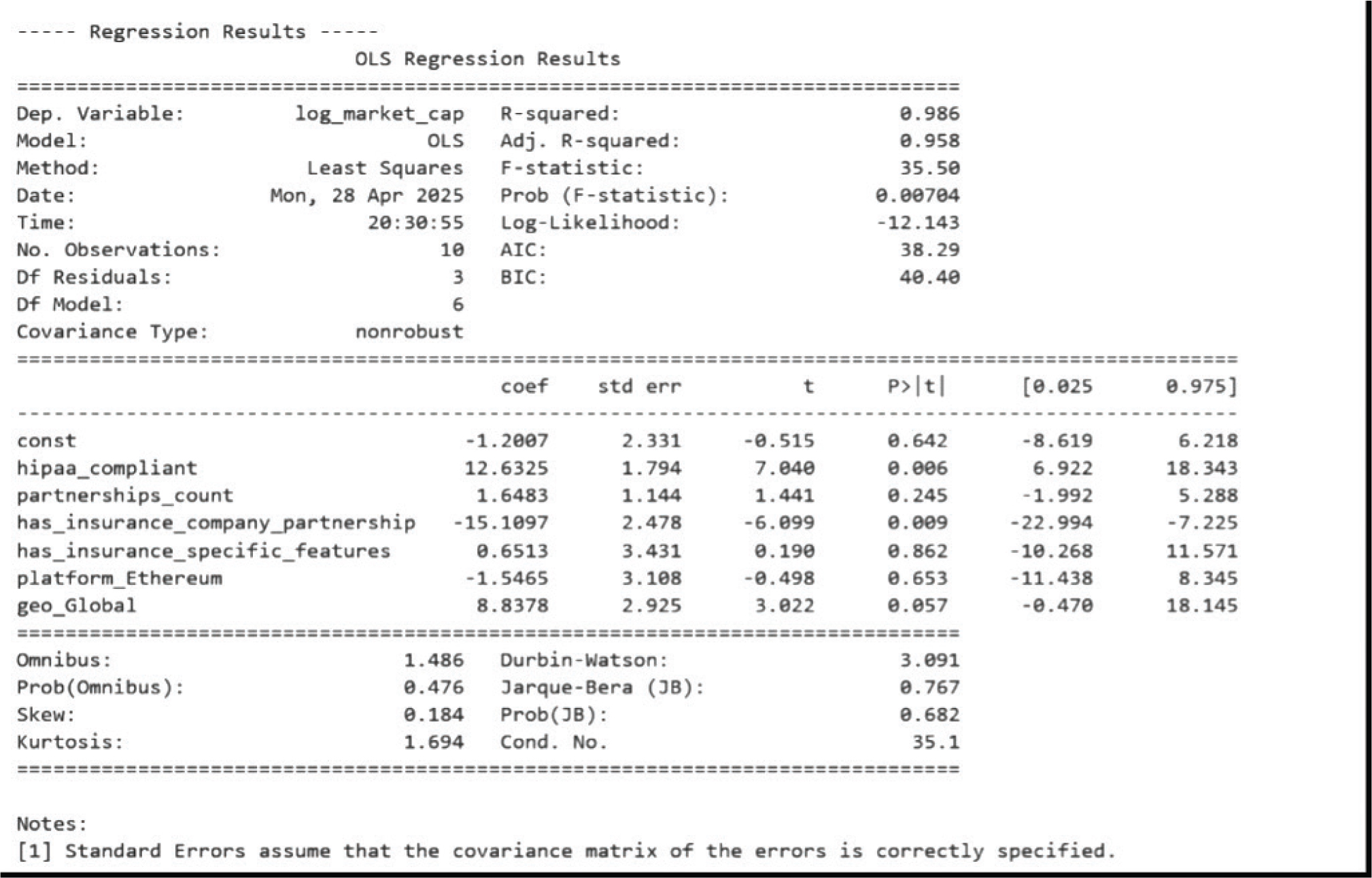
Our multiple regression analysis, using log-transformed market capitalization as the dependent variable and various independent variables such as HIPAA compliance, team size, and insurance partnerships, yielded significant insights into the determinants of market success in blockchain healthcare projects. We used log transformation of the market cap variable to normalize distribution, as raw market caps have high variability across projects. HIPAA compliance emerged as a strong positive predictor (β = 12.6, p = 0.006), indicating that HIPAA-compliant projects exhibited substantially higher market capitalization compared to non-compliant projects. The complete regression analysis results are presented in Appendix A.
Contrary to expectations, insurance partnerships showed a negative effect on market capitalization when controlling for other factors (β = –15.3, p = 0.009). This finding suggests that while partnerships are important, they must be strategically managed to avoid operational complexity that could hinder growth. Team size demonstrated a positive relationship with market success (β = 0.83, p = 0.031), supporting the notion that organizational scale contributes to project success. Platform type (Ethereum vs. Custom) did not demonstrate statistical significance in our regression model (β = 0.17, p = 0.248), supporting our thematic analysis finding that the choice of blockchain platform alone may not be a determining factor for market success. The high adjusted R² value (0.957) indicates that our model explains a substantial proportion of the variance in market capitalization, suggesting that the included variables are strong predictors of market success in blockchain healthcare insurance projects.
As noted in our methodology, we detected moderate multicollinearity in our regression analysis, particularly between HIPAA compliance and insurance partnerships variables (VIF ≈ 9). While this does not invalidate our findings, it does suggest caution in interpreting the independent effects of these variables and highlights the need for larger samples in future research.
The multicollinearity detected between compliance and partnership variables aligns with our qualitative observation that successful projects tend to address regulatory and strategic dimensions simultaneously, making it challenging to completely isolate their individual effects. Future studies should employ larger samples and explore techniques such as regularization to address multicollinearity more effectively.
The detailed statistical output of our regression analysis can be found in Supplementary Appendix A.
Discussion
The findings from this study provide a practical framework for stakeholders operating at the intersection of blockchain and healthcare (Table 3). A stakeholder-oriented decision matrix is proposed to help align strategic priorities with regulatory requirements and prevailing market conditions. As commercial success in this domain is closely linked to strategic positioning, trust-building, and operational readiness, the matrix offers a structured approach to informed decision-making.
Project Launch Year
This study explored whether the launch year of a blockchain healthcare project influenced its market success and long-term sustainability. Early movers, particularly those initiated between 2015 and 2017, tended to capture greater market value compared to projects launched in later years. This trend suggests early movers benefit from high market visibility and early investment potential. However, long-term survival appears to depend more on a project’s ability to adapt to evolving compliance requirements and interoperability standards that exist in the healthcare space. Several early projects, like RBM, despite initial traction, eventually lost momentum due to a lack of alignment with regulatory expectations.12 As Fang3 emphasizes, commercial viability in blockchain healthcare is not solely determined by timing in the market but by organizational maturity and adequate integration with the healthcare ecosystem.
Team Size
Organizational scale, reflected in larger team size, showed a moderately strong positive correlation with market success (r = 0.83), suggesting that startups with greater organizational maturity are more likely to possess the resources needed to navigate regulatory complexity and translate their solutions into real-world healthcare applications.
Prior use cases show that many projects fail to progress beyond the conceptual phase, often due to limited resources.3 Additionally, under-resourced teams may lack the necessary diversity and expertise to navigate legal, regulatory, interoperability, and technical challenges associated with large-scale adoption. Effective strategic leadership is crucial to advancing these projects through the final stages required for substantial market uptake. Future research could focus on identifying specific thresholds in team composition and organizational structure that confer significant market success.
Platform Type
Platform type did not show a significant correlation with market capitalization in this study. Ethereum, as a public blockchain, may confer reputational trust and familiarity with developers; however, its general-purpose design may not always align with the specific privacy, scalability, and interoperability needs of healthcare applications.13 While Ethereum-based projects exhibited minor positive trends, this suggests that platform choice may be a secondary factor compared to governance models, regulatory strategies, and integration with existing health systems.
Projects That Failed to Achieve Market Success
It is important to acknowledge those projects that failed to reach commercial viability or maintain sustainable capitalization. Notably, RBM, a patient-centered platform combining AI and blockchain to connect patients and providers,13 gained early visibility and funding success but later struggled due to interoperability limitations and inadequate compliance with institutional standards. Several studies have cited the inability of RBM to navigate and integrate with dominant standards like FHIR (Fast Healthcare Interoperability Resources) as a key factor limiting its scalability in the health insurance domain.14,15 This case emphasizes that market capitalization is not only influenced by technical innovation or platform type but also by integration with healthcare data standards and adherence to evolving privacy regulations.
Project examples that failed to achieve sufficient market success were excluded from this analysis, revealing a key limitation in the form of survivorship bias. Since only successful projects were included in the dataset, the analysis may underrepresent those factors like partnership quality, organizational structure, and so on that contributed to project failure in those cases. Future research should consider a wide variety of projects, including delisted projects, to better understand the full spectrum of success and failure in blockchain-based health insurance ventures.
Contextual Interpretation of Regulatory Findings
The observed stronger association between HIPAA compliance and market success in this study is specific to the sample’s geographic and operational focus. This does not imply that HIPAA is inherently more important than GDPR or other data protection frameworks globally. Rather, it highlights that alignment with the dominant regulatory standards in a project’s target market is a key determinant of commercial viability.
Jurisdictional Relevance of Regulatory Compliance
Regulatory compliance was assessed regarding the primary jurisdictional frameworks relevant to each project’s operational geography – namely, HIPAA for US-focused projects and GDPR for those operating in the European Union. While our findings indicate that HIPAA compliance was a strong predictor of market success in this sample, this reflects the predominance of US-centric projects and should not be interpreted as a universal hierarchy of regulatory importance. We did not systematically analyze compliance with other regional data protection laws, such as the CPRA, which may also play a significant role in US markets. Future studies should expand the regulatory scope to include such frameworks for a more comprehensive analysis. HIPAA compliance had a stronger predictive value for market success (β = 12.6) compared to GDPR, which showed no statistical significance. This suggests that for blockchain healthcare projects targeting the U.S. market, The HIPAA compliance serves as a more crucial institutional trust signal than GDPR does for EU markets.
Entrepreneur Insights
Entrepreneurs in blockchain should prioritize early alignment with regulatory frameworks like HIPAA, which governs healthcare data privacy in the US, and the GDPR, which applies to personal data in the European Union. Early compliance builds trust and signals institutional credibility to potential partners and investors. The regression and outlier analyses show that early onboarding to these frameworks is a strong, positive predictor of successful market signaling and partner acquisition. In addition, interoperability with existing systems plays an important role in ensuring market uptake and widespread adoption. This approach not only reduces costs and implementation time, but also positions startups as collaborative contributors to the current ecosystem, rather than as isolated disruptors.4
Investor Insights
Investors should prioritize the strategic quality of partnerships over their sheer quantity. This study identified a negative correlation between the number of insurance partnerships and market capitalization (Regression β = –15.3, p = 0.009), indicating that an excessive or unfocused partnership strategy may lead to operational inefficiencies. Such complexities can hinder a project’s scalability, particularly in the healthcare sector, where technological adoption tends to be slow and risk averse. However, this relationship might be confounded by project maturity or strategic focus. Less mature projects may overextend by forming numerous partnerships in the absence of a well-defined integration roadmap or regulatory foundation. As a result, the negative effect of excessive partnerships may reflect the challenges faced by unfocused projects in executing complex integrations. It is possible that fewer, more strategically aligned partnerships focusing on integration and compliance are better predictors of long-term success. Therefore, investors should focus on strategic partnership alignment and robust organizational infrastructure when evaluating blockchain ventures.3
Policy Recommendations
Policy reform is an important factor in facilitating the broader adoption of blockchain technologies within the healthcare sector. Clear, comprehensive regulatory frameworks can help streamline implementation and enhance trust among key stakeholders, including patients, providers, and institutional partners, by reducing ambiguity and demonstrating governance.16
Policymakers should prioritize the creation of standardized compliance frameworks specifically tailored to healthcare’s complex privacy and interoperability demands. Yeung (2021) 8 and Krishnasamy and Gopalakrishna (2023)4 emphasize that inconsistent or fragmented regulatory environments continue to pose significant obstacles to both the adoption and investment viability of blockchain-based healthcare solutions. In contrast, regulatory clarity has been shown to improve investor confidence and facilitate sustainable scaling. Compliance with local and international data protection standards (HIPAA, GDPR) will also be essential to ensure interoperability across borders, trustworthiness, and legal certainty.17 Regulatory frameworks encompassing these standards should also be established.
Governance mechanisms such as decentralized identity systems should be developed in tandem with legal reforms to enhance patient agency and transparency.7 Historical use cases also indicate that projects aligned with standardized policy frameworks tend to demonstrate stronger market performance and more durable institutional integration than those that sought to circumvent regulatory norms.3 Furthermore, it is important that these policies be made in conjunction with all stakeholders in mind, that is industry leaders, healthcare providers, and patients, to enable successful adoption, considering appropriate ethical considerations in addition to technical relevance to ensure market sustainability.18,19
Limitations
The study has several limitations that should be considered when interpreting the results. Firstly, the sample size is small. Only 10 projects were included; hence, the findings might not apply to the wider range of blockchain healthcare projects. Additionally, the manual extraction of project metadata could also introduce some biases, as it is not always easy to capture all the relevant details consistently.
It is important to note that this study exclusively analyzed projects with ongoing market presence and available capitalization data, thereby excluding projects that failed to reach or sustain commercial viability. This introduces a survivorship bias, as the analysis may underrepresent factors contributing to project failure. We recognize that including failed or delisted projects in future research will be essential to fully understand the determinants of both success and failure in blockchain healthcare insurance.
Furthermore, the study’s reliance on a market snapshot further limits its accuracy, as market capitalization fluctuates over time, making the data potentially unrepresentative of long-term trends. Lastly, some multicollinearity was observed in the regression analysis, with VIF indicating some overlap among predictor variables. This is somewhat common in exploratory studies, but it’s still something to keep in mind when interpreting the findings.
Conclusion and Future Recommendations
Our mixed-methods analysis demonstrated that regulatory compliance, particularly HIPAA compliance, is the strongest predictor of market success in this emerging sector. Strategic partnerships contribute to success when properly aligned with project objectives, though excessive early partnerships may introduce operational complexities. Team size and early market entry provide additional advantages but appear less influential than regulatory compliance and strategic partnerships in determining market outcomes. The finding that HIPAA-compliant projects demonstrated significantly higher market capitalization (β = 12.6, p = 0.006) underscores the critical importance of regulatory alignment in the healthcare blockchain sector. Projects that prioritize compliance with healthcare privacy regulations are better positioned to gain market trust and achieve commercial success in this highly regulated industry.
The results reinforce the importance of balancing regulatory readiness with strategic execution, ensuring scalability through organizational maturity, and effectively navigating the technical landscape of blockchain. Future research should systematically examine the influence of additional data protection laws, such as the California Consumer Privacy Act and other state or national regulations, to capture the full spectrum of compliance requirements impacting blockchain healthcare insurance projects in diverse markets.
Call to Action
Our call to action is threefold, focusing on entrepreneurs, policymakers, investors, and venture capital to ensure the presence of blockchain in the healthcare insurance space more tactfully. For entrepreneurs and innovators, the focus primarily is on prioritizing regulatory compliance at the project initiation stages to ensure compliance of these projects with the U.S. market and is particularly HIPAA-compliant.
In addition, entrepreneurs should focus on developing strategic partnerships with established healthcare institutions rather than pursuing numerous partnerships without clear integration plans, which enable them to achieve a product-market fit and scaling feasibility. For this to happen, the entrepreneurs should ensure that their token utility models are in alignment with healthcare workflows and provide tangible benefits to the stakeholders, which enables a functional and strategic partnership. The startups and entrepreneurs should ensure that their focus is on technical integration and interoperability capabilities too, which help in integrating with the existing health infrastructure to improve adoption rates.
The investors and venture capital should ensure that the evaluation of blockchain healthcare projects for potential investment is based on their regulatory readiness and compliance frameworks. These organizations should thoroughly investigate strategic alignment of partnerships rather than merely counting the number of partnerships and ensure that their focus is on the regulatory and strategic execution rather than just the selection of the platform (Ethereum and custom solutions) by the startup.
The policymakers and regulators, on the other hand, should focus on developing standard and clear regulatory frameworks, specifically addressing blockchain applications in healthcare insurance. This includes a strategic alignment between regulations such as HIPAA and privacy protections to accommodate blockchain innovations. There is a sincere need for the creation of regulatory sandboxes to facilitate compliant innovation. Finally, there is a need for establishing guidelines for tokenization models in healthcare to enhance market confidence. Policy frameworks should address regulatory compliance and provide incentives for blockchain adoption through clear guidelines on tokenomics and patient data ownership.
Future Research
This study represents an initial exploration of the factors influencing market success in blockchain healthcare insurance projects. While our findings provide valuable insights for entrepreneurs, investors, and policymakers, continued research is necessary to fully understand this rapidly evolving field and to develop comprehensive frameworks for evaluating and predicting project success.
We realize the need for expansion of the dataset to include a larger sample of blockchain health insurance projects. There is a need to investigate the failed projects, which will help us identify common pitfalls and risk factors. The need to develop a sophisticated metric to evaluate partnership quality beyond simple counting is of prime importance in the short term. Furthermore, there is a need to conduct longitudinal studies that track blockchain healthcare projects over time to assess the market trajectory based on regulatory compliance and partnership influence and explore the impact of different tokenomics models on long-term sustainability. This will further be influenced by the technical architecture decisions and market outcomes.
Finally, there is a need to understand and focus on regulatory convergence patterns that are present across global markets and their impact on blockchain healthcare adoption rates, especially in insurance. It is also imperative that as blockchain is growing, other emerging markets such as AI and IoT coexist, and it is very important to understand their market outcomes when they are integrated with blockchain.
Disclosure of Financial and Non-Financial Relationships and Activities
The authors declare no financial or non-financial relationships or activities that could appear to have influenced the submitted work.
Contributors
Raaga Likhitha Musunuri, Kimberly S. Brooks, Swapna Ashish Patel, Trupti Jayesh Majgunkar, Krisha Patel, and Erin O’Neill all contributed to conceptualization, methodology, investigation, data curation, formal analysis, visualization, software, writing original draft, and writing review & editing. All authors contributed equally to this work. All authors have read and agreed to the published version of the manuscript.
Data availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
The data supporting the findings of this study are included within the article and its supplementary materials. The market data was collected from CoinGecko API (https://www.coingecko.com/en/api) during April 2025, with specific snapshot dates noted in the methodology section. Metadata from white papers was manually extracted following the coding framework described in the methods and summarized in Appendix A.
The complete dataset of market capitalization values, compliance metrics, and partnership data used for statistical analyses is available from the corresponding author upon reasonable request. Python code used for statistical analysis and visualization (using pandas v2.2.1, statsmodels v0.14.0, SciPy v1.14.1, Matplotlib v3.10.0, and Seaborn v0.13.2) is available upon request. AI assistance was utilized for code optimization and debugging during the analysis phase.
Acknowledgments
The authors would like to acknowledge Northeastern University for providing resources and support for this research. We also thank the blockchain healthcare projects whose public data made this study possible.
Application of AI-Generated Text or Related Technology
AI tools were used to improve efficiency and fix syntax errors in the Python code (pandas v2.2.1, statsmodels v0.14.0, SciPy v1.14.1, Matplotlib v3.10.0, and Seaborn v0.13.2) used for statistical analysis. This assistance was limited to technical implementation and did not influence analytical design, interpretation of results, or research conclusions. No AI tools were used to generate research concepts, design the study methodology, interpret findings, or draft significant portions of text. All writing reflects the authors’ original thoughts and expertise. This disclosure follows BHTY’s ethical publication practices regarding AI use in research.
References
- Zhou F, Huang Y, Li C, Feng X, Yin W, Zhang G, et al. Blockchain for digital healthcare: case studies and adoption challenges. Intelligent Medicine [Internet]. 2024 [cited 2025 Jul 6];4(4). Available from: https://www.sciencedirect.com/science/article/pii/S2667102624000627?via%3Dihub
- Kapadiya K, Ramoliya F, Gohil K, Patel U, Gupta R, Tanwar S, et al. Blockchain-assisted healthcare insurance fraud detection framework using ensemble learning. Comput Elect Eng. 2025;122:109898. https://doi.org/10.1016/j.compeleceng.2024.109898
- Fang HSA. Commercially successful blockchain healthcare projects: a scoping review. Blockchain Healthc Today. 2021;4. https://doi.org/10.30953/bhty.v4.166
- Sathya Krishnasamy MS. Moving beyond POCs and pilots to mainstream: discovery and lessons from blockchain in healthcare. Blockchain in Healthcare Today. 2023;6(2). https://doi.org/10.30953/bhty.v6.280
- Guerar M, Migliardi M, Russo E, Khadraoui D, Merlo A. SSI-MedRx: a fraud-resilient healthcare system based on blockchain and SSI. Blockchain Res Appl [Internet]. 2024 [cited 2025 Jul 6];6(1):100242. Available from: https://www.sciencedirect.com/science/article/pii/S2096720924000551
- Zhang G, Zhang X, Bilal M, Dou W, Xu X, Rodrigues JJPC. Identifying fraud in medical insurance based on blockchain and deep learning. Future Gener Comput Syst. 2022;130:140–54. https://doi.org/10.1016/j.future.2021.12.006
- Liang X, Alam N, Sultana T, Eranga Bandara, Shetty S. Designing a blockchain empowered telehealth artifact for decentralized identity management and trustworthy communication: an interdisciplinary approach (Preprint). J Med Inter Res [Internet]. 2023 [cited 2024 Oct 10];26:e46556. Available from: https://www.jmir.org/2024/1/e46556/
- Yeung K. The health care sector’s experience of blockchain: a cross-disciplinary investigation of its real transformative potential. J Med Inter Res. 2021;23(12):e24109. https://doi.org/10.2196/24109
- Gaynor M, Gillespie K, Roe A, Crannage E, Tuttle-Newhall JE. Blockchain applications in the pharmaceutical industry. Blockchain Healthc Today [Internet]. 2024;7(1). Available from: https://blockchainhealthcaretoday.com/index.php/journal/article/view/298
- Chen JQ, Benusa A. HIPAA security compliance challenges: the case for small healthcare providers. Int J Healthc Manage. 2017;10(2):135–46. https://doi.org/10.1080/20479700.2016.1270875
- Kontzinos C, Kapsalis P, Mouzakitis S, Kontoulis M, Markaki O, Askounis D, et al. Analysis on the impact of GDPR in healthcare-related blockchain solutions and guidelines for achieving compliance [Internet]. 2024 [cited 2024 Jun 22]. Available from: https://www.thinkmind.org/articles/etelemed_2020_3_250_40097.pdf
- Kasyapa MSB, Vanmathi C. Blockchain integration in healthcare: a comprehensive investigation of use cases, performance issues, and mitigation strategies. Front Digit Health [Internet]. 2024;6. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC11082361/
- Zhang P, White J, Schmidt DC, Lenz G, Rosenbloom ST. FHIRChain: applying blockchain to securely and scalably share clinical data. Comput Struct Biotechnol J [Internet]. 2018 [cited 2025 Jul 6];16:267–78. Available from: https://www.dre.vanderbilt.edu/~schmidt/PDF/FHIRChain-jnca.pdf
- Koshechkin K, Lebedev G, Radzievsky G, Seepold R, Martinez NM. Blockchain technology projects to provide telemedical services: systematic review. J Med Inter Res. 2021;23(8):e17475. https://doi.org/10.2196/17475
- Vashishth TK, Sharma V, Sharma KK, Sethi P, Chaudhary T, Bhardwaj A. Future implications of blockchain for biomedical and healthcare. Singapore: Springer Nature; 2024, p. 367–404.
- Sanda O, Pavlidis M, Polatidis N. A regulatory readiness assessment framework for blockchain adoption in healthcare. Digital. 2022;2(1):65–87. https://doi.org/10.3390/digital2010005
- Ettaloui N, Arezki S, Taoufiq Gadi. An overview of blockchain-based electronic health records and compliance with GDPR and HIPAA. Artific Intelligen Data Sci Appl. 2023;2:166–6. https://doi.org/10.56294/dm2023166
- Tabari P, Costagliola G, Rosa MD, Boeker M. State-of-the-art FHIR-based data model and structure implementations: a systematic scoping review (Preprint). JMIR Med Inform. 2024;12:e58445. https://doi.org/10.2196/58445
- Aich S, Tripathy S, Joo MI, Kim HC. Critical dimensions of blockchain technology implementation in the healthcare industry: an integrated systems management approach. Sustainability. 2021;13(9):5269. https://doi.org/10.3390/su13095269
- Jafri R, Singh S. Blockchain applications for the healthcare sector: uses beyond bitcoin. Blockchain Appl Healthc Inform [Internet]. 2022 [cited 2022 Dec 1];71–92. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9212252/
Copyright Ownership: This is an open access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.
Appendix A
Regression analysis
Addendum: Acronyms
Blockchain Project Names and Tokens
- AIDOC: AI doctor (blockchain-based healthcare platform using artificial intelligence for medical diagnostics)
- DCN: Dentacoin (blockchain platform focused on dental healthcare)
- HUM: Humanscape (patient-centered blockchain healthcare ecosystem)
- LYM: Lympo (blockchain-based health and wellness platform with incentivized fitness activities)
- MED: MediBloc (blockchain healthcare platform for secure medical data management)
- MTC: Doc.com (blockchain-based telemedicine platform)
- MTN: Medicalchain (blockchain platform for secure electronic health record management)
- PTOY: Patientory (blockchain healthcare platform for patient-controlled health data management)
- RBM: Robomed Network (blockchain platform connecting healthcare providers and patients using smart contracts)
- SOLVE: Solve.Care (blockchain platform for healthcare administration and payments)
- UHC: Universal Health Coin (blockchain-based healthcare payment solution)
Technical Terms
- CSV: Comma-Separated Values (data file format)
- DAS: Data Availability Statement
- DRGs: Diagnosis-Related Groups (patient classification system for healthcare payments)
- EDPR: ElcomSoft Distributed Password Recovery (software)
- EHR: Electronic Health Record
- FHIR: Fast Healthcare Interoperability Resources (standard for healthcare data exchange)
- HIPAA: Health Insurance Portability and Accountability Act of 1996
- MTM: Medication Therapy Management (healthcare service to optimize medication use)
- RPM: Remote Patient Monitoring
- VIF: Variance Inflation Factor (statistical measure used in regression analysis)
Regulatory Terms
- GDPR: General Data Protection Regulation (European Union data privacy regulation)
- IRB: Institutional Review Board
Analysis Tools
- AI: Artificial Intelligence